what is insulin? how does it works ?

INSULIN
Insulin (/ˈɪn.sjʊ.lɪn/, from Latin insula, ‘island’) is a peptide hormone produced by beta cells of the pancreatic islets; it is considered to be the main anabolic hormone of the body. It regulates the metabolism of carbohydrates, fats, and protein by promoting the absorption of glucose from the blood into the liver, fat, and skeletal muscle cells. In these tissues, the absorbed glucose is converted into either glycogen via glycogenesis or fats (triglycerides) via lipogenesis, or, in the case of the liver, into both. Glucose production and secretion by the liver are strongly inhibited by high concentrations of insulin in the blood. Circulating insulin also affects the synthesis of proteins in a wide variety of tissues. It is therefore an anabolic hormone, promoting the conversion of small molecules in the blood into large molecules inside the cells. Low insulin levels in the blood have the opposite effect by promoting widespread catabolism, especially of reserve body fat.
Beta cells are sensitive to blood sugar levels so they secrete insulin into the blood in response to a high level of glucose, and inhibit the secretion of insulin when glucose levels are low. Insulin enhances glucose uptake and metabolism in the cells, thereby reducing blood sugar levels. Their neighboring alpha cells, by taking their cues from the beta cells, secrete glucagon into the blood in the opposite manner: increased secretion when blood glucose is low, and decreased secretion when glucose concentrations are high. Glucagon increases blood glucose levels by stimulating glycogenolysis and gluconeogenesis in the liver. The secretion of insulin and glucagon into the blood in response to the blood glucose concentration is the primary mechanism of glucose homeostasis.
Decreased or loss of insulin activity results in diabetes mellitus, a condition of high blood sugar level (hyperglycemia). There are two types of the disease. In type 1 diabetes mellitus, the beta cells are destroyed by an autoimmune reaction so that insulin can no longer be synthesized or secreted into the blood In type 2 diabetes mellitus, the destruction of beta cells is less pronounced than in type 1 diabetes, and is not due to an autoimmune process. Instead, there is an accumulation of amyloid in the pancreatic islets, which likely disrupts their anatomy and physiology. The pathogenesis of type 2 diabetes is not well understood but a reduced population of islet beta-cells, reduced secretory function of islet beta-cells that survive, and peripheral tissue insulin resistance is known to be involved.[7] Type 2 diabetes is characterized by increased glucagon secretion which is unaffected by, and unresponsive to the concentration of blood glucose. But insulin is still secreted into the blood in response to the blood glucose. As a result, glucose accumulates in the blood.
The human insulin protein is composed of 51 amino acids and has a molecular mass of 5808 Da. It is a heterodimer of an A-chain and a B-chain, which are linked together by disulfide bonds. Insulin’s structure varies slightly between species of animals. Insulin from animal sources differs somewhat in effectiveness (in carbohydrate metabolism effects) from human insulin because of these variations. Porcine insulin is especially close to the human version and was widely used to treat type 1 diabetics before human insulin could be produced in large quantities by recombinant DNA technologies.
Insulin was the first peptide hormone discovered. Frederick Banting and Charles Herbert Best, working in the laboratory of J.J.R. Macleod at the University of Toronto, were the first to isolate insulin from dog pancreas in 1921. Frederick Sanger sequenced the amino acid structure in 1951, which made insulin the first protein to be fully sequenced. The crystal structure of insulin in the solid state was determined by Dorothy Hodgkin in 1969. Insulin is also the first protein to be chemically synthesized and produced by DNA recombinant technology. It is on the WHO Model List of Essential Medicines, the most important medications needed in a basic health system.
Gene
The preproinsulin precursor of insulin is encoded by the INS gene, which is located on chromosome 11p15.5.
Alleles
A variety of mutant alleles with changes in the coding region have been identified. A read-through gene, INS-IGF2, overlaps with this gene at the 5′ region and with the IGF2 gene at the 3′ region.
Structure
The structure of insulin. The left side is a space-filling model of the insulin monomer, believed to be biologically active. Carbon is green, hydrogen white, oxygen red, and nitrogen blue. On the right side is a ribbon diagram of the insulin hexamer, believed to be the stored form. A monomer unit is highlighted with the A chain in blue and the B chain in cyan. Yellow denotes disulfide bonds, and magenta spheres are zinc ions.
Contrary to an initial belief that hormones would be generally small chemical molecules, as the first peptide hormone known for its structure, insulin was found to be quite large. A single protein (monomer) of human insulin is composed of 51 amino acids and has a molecular mass of 5808 Da. The molecular formula of human insulin is C257H383N65O77S6. It is a combination of two peptide chains (dimer) named an A-chain and a B-chain, which are linked together by two disulfide bonds. The A-chain is composed of 21 amino acids, while the B-chain consists of 30 residues. The linking (interchain) disulfide bonds are formed at cysteine residues between the positions A7-B7 and A20-B19. There is an additional (intrachain) disulfide bond within the A-chain between cysteine residues at positions A4 and A11. The A-chain exhibits two α-helical regions at A1-A8 and A12-A19 which are antiparallel; while the B chain has a central α -helix (covering residues B9-B19) flanked by the disulfide bond on either side and two β-sheets (covering B7-B10 and B20-B23).
The amino acid sequence of insulin is strongly conserved and varies only slightly between species. Bovine insulin differs from humans in only three amino acid residues and porcine insulin in one. Even insulin from some species of fish is similar enough to humans to be clinically effective in humans. Insulin in some invertebrates is quite similar in sequence to human insulin and has similar physiological effects. The strong homology seen in the insulin sequence of diverse species suggests that it has been conserved across much of animal evolutionary history. The C-peptide of proinsulin, however, differs much more among species; it is also a hormone, but a secondary one.
Insulin is produced and stored in the body as a hexamer (a unit of six insulin molecules), while the active form is the monomer.
Synthesis
Insulin is produced in the pancreas and the Brockmann body (in some fish), and released when any of several stimuli are detected. These stimuli include the rise in plasma concentrations of amino acids and glucose resulting from the digestion of food. Carbohydrates can be polymers of simple sugars or the simple sugars themselves. If the carbohydrates include glucose, then that glucose will be absorbed into the bloodstream, and the blood glucose level will begin to rise. In target cells, insulin initiates signal transduction, which has the effect of increasing glucose uptake and storage. Finally, insulin is degraded, terminating the response.
Insulin undergoes extensive posttranslational modification along the production pathway. Production and secretion are largely independent; prepared insulin is stored awaiting secretion. Both C-peptide and mature insulin are biologically active. Cell components and proteins in this image are not to scale.
In mammals, insulin is synthesized in the pancreas within the beta cells. One million to three million pancreatic islets form the endocrine part of the pancreas, which is primarily an exocrine gland. The endocrine portion accounts for only 2% of the total mass of the pancreas. Within the pancreatic islets, beta cells constitute 65–80% of all the cells.[
Insulin consists of two polypeptide chains, the A- and B- chains, linked together by disulfide bonds. It is however first synthesized as a single polypeptide called preproinsulin in beta cells. Preproinsulin contains a 24-residue signal peptide which directs the nascent polypeptide chain to the rough endoplasmic reticulum (RER). The signal peptide is cleaved as the polypeptide is translocated into the lumen of the RER, forming proinsulin. In the RER the proinsulin folds into the correct conformation and 3 disulfide bonds are formed. About 5–10 min after its assembly in the endoplasmic reticulum, proinsulin is transported to the trans-Golgi network (TGN) where immature granules are formed. Transport to the TGN may take about 30 minutes.
Proinsulin undergoes maturation into active insulin through the action of cellular endopeptidases known as prohormone convertases (PC1 and PC2), as well as the exoprotease carboxypeptidase E. The endopeptidases cleave at 2 positions, releasing a fragment called the C-peptide, and leaving 2 peptide chains, the B- and A- chains, linked by 2 disulfide bonds. The cleavage sites are each located after a pair of basic residues (lysine-64 and arginine-65, and arginine-31 and −32). After cleavage of the C-peptide, these 2 pairs of basic residues are removed by the carboxypeptidase. The C-peptide is the central portion of proinsulin, and the primary sequence of proinsulin goes in the order “B-C-A” (the B and A chains were identified on the basis of mass and the C-peptide was discovered later).
The resulting mature insulin is packaged inside mature granules waiting for metabolic signals (such as leucine, arginine, glucose, and mannose) and vagal nerve stimulation to be exocytosed from the cell into the circulation.
The endogenous production of insulin is regulated in several steps along the synthesis pathway:
- A transcription from the insulin gene
- In mRNA stability
- At the mRNA translation
- In the posttranslational modifications
Insulin and its related proteins are produced inside the brain, and reduced levels of these proteins are linked to Alzheimer’s disease.
Insulin release is stimulated also by beta-2 receptor stimulation and inhibited by alpha-1 receptor stimulation. In addition, cortisol, glucagon, and growth hormone antagonize the actions of insulin during times of stress. Insulin also inhibits fatty acid release by hormone-sensitive lipase in adipose tissue.
Release
Beta cells in the islets of Langerhans release insulin in two phases. The first-phase release is rapidly triggered in response to increased blood glucose levels and lasts about 10 minutes. The second phase is a sustained, slow release of newly formed vesicles triggered independently of sugar, peaking in 2 to 3 hours. Reduced first-phase insulin release may be the earliest detectable beta-cell defect predicting the onset of type 2 diabetes. First-phase release and insulin sensitivity are independent predictors of diabetes.
The description of the first phase release is as follows:
- Glucose enters the β-cells through the glucose transporters, GLUT2. These glucose transporters have a relatively low affinity for glucose, ensuring that the rate of glucose entry into the β-cells is proportional to the extracellular glucose concentration (within the physiological range). At low blood sugar levels, very little glucose enters the β-cells; at high blood glucose concentrations, large quantities of glucose enter these cells.
- The glucose that enters the β-cell is phosphorylated to glucose-6-phosphate (G-6-P) by glucokinase (hexokinase IV) which is not inhibited by G-6-P in the way that the hexokinases in other tissues (hexokinase I – III) are affected by this product. This means that the intracellular G-6-P concentration remains proportional to the blood sugar concentration.
- Glucose-6-phosphate enters the glycolytic pathway and then, via the pyruvate dehydrogenase reaction, into the Krebs cycle, where multiple, high-energy ATP molecules are produced by the oxidation of acetyl CoA (the Krebs cycle substrate), leading to a rise in the ATP: ADP ratio within the cell.
- An increased intracellular ATP: ADP ratio closes the ATP-sensitive SUR1/Kir6.2 potassium channel (see sulfonylurea receptor). This prevents potassium ions (K+) from leaving the cell by facilitated diffusion, leading to a buildup of intracellular potassium ions. As a result, the inside of the cell becomes less negative than the outside, leading to the depolarization of the cell surface membrane.
- Upon depolarization, voltage-gated calcium ion (Ca2+) channels open, allowing calcium ions to move into the cell by facilitated diffusion.
- The cytosolic calcium ion concentration can also be increased by calcium release from intracellular stores via activation of ryanodine receptors.
- The calcium ion concentration in the cytosol of the beta cells can also, or additionally, be increased through the activation of phospholipase C resulting from the binding of an extracellular ligand (hormone or neurotransmitter) to a G protein-coupled membrane receptor. Phospholipase C cleaves the membrane phospholipid, phosphatidylinositol 4,5-bisphosphate, into inositol 1,4,5-trisphosphate and diacylglycerol. Inositol 1,4,5-trisphosphate (IP3) then binds to receptor proteins in the plasma membrane of the endoplasmic reticulum (ER). This allows the release of Ca2+ ions from the ER via IP3-gated channels, which raises the cytosolic concentration of calcium ions independently of the effects of a high blood glucose concentration. Parasympathetic stimulation of the pancreatic islets operates via this pathway to increase insulin secretion into the blood.
- The significantly increased amount of calcium ions in the cells’ cytoplasm causes the release into the blood of previously synthesized insulin, which has been stored in intracellular secretory vesicles.
This is the primary mechanism for the release of insulin. Other substances known to stimulate insulin release include the amino acids arginine and leucine, the parasympathetic release of acetylcholine (acting via the phospholipase C pathway), sulfonylurea, cholecystokinin (CCK, also via phospholipase C), and the gastrointestinally derived incretins, such as glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic peptide (GIP).
The release of insulin is strongly inhibited by norepinephrine (noradrenaline), which leads to increased blood glucose levels during stress. It appears that the release of catecholamines by the sympathetic nervous system has conflicting influences on insulin release by beta cells because insulin release is inhibited by α2-adrenergic receptors and stimulated by β2-adrenergic receptors. The net effect of norepinephrine from sympathetic nerves and epinephrine from adrenal glands on insulin release is inhibition due to the dominance of the α-adrenergic receptors.
When the glucose level comes down to the usual physiologic value, insulin release from the β-cells slows or stops. If the blood glucose level drops lower than this, especially to dangerously low levels, the release of hyperglycemic hormones (most prominent glucagon from the islet of Langerhans alpha cells) forces the release of glucose into the blood from the liver glycogen stores, supplemented by gluconeogenesis if the glycogen stores become depleted. By increasing blood glucose, the hyperglycemic hormones prevent or correct life-threatening hypoglycemia.
Evidence of impaired first-phase insulin release can be seen in the glucose tolerance test, demonstrated by a substantially elevated blood glucose level 30 minutes after the ingestion of a glucose load (75 gm, followed by a slow drop over the next 100 minutes, to remain above 120 mg/100 ml after two hours after the start of the test. In a normal person, the blood glucose level is corrected (and may even be slightly over-corrected) by the end of the test. An insulin spike is a ‘first response’ to blood glucose increase, this response is individual and dose-specific although it was always previously assumed to be food type-specific only.
Oscillations
Even during digestion, in general, one or two hours following a meal, insulin release from the pancreas is not continuous, but oscillates over 3–6 minutes, changing from generating a blood insulin concentration of more than about 800 pmol/l to less than 100 pmol/l (in rats). This is thought to avoid the downregulation of insulin receptors in target cells and to assist the liver in extracting insulin from the blood. This oscillation is important to consider when administering insulin-stimulating medication since it is the oscillating blood concentration of insulin release, which should, ideally, be achieved, not a constant high concentration. This may be achieved by delivering insulin rhythmically to the portal vein, by light-activated delivery, or by islet cell transplantation to the liver.
Blood insulin level
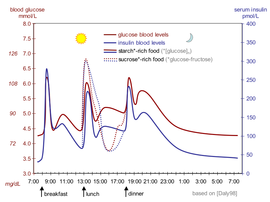
The idealized diagram shows the fluctuation of blood sugar (red) and the sugar-lowering hormone insulin (blue) in humans during a day containing three meals. In addition, the effect of a sugar-rich versus a starch-rich meal is highlighted.
The blood insulin level can be measured in international units, such as µIU/mL, or in molar concentration, such as pmol/L, where 1 µIU/mL equals 6.945 pmol/L. A typical blood level between meals is 8–11 μIU/mL (57–79 pmol/L).
Signal transduction
The effects of insulin are initiated by its binding to a receptor present in the cell membrane. The receptor molecule contains an α- and β subunits. Two molecules are joined to form what is known as a homodimer. Insulin binds to the α-subunits of the homodimer, which faces the extracellular side of the cells. The β subunits have tyrosine kinase enzyme activity which is triggered by insulin binding. This activity provokes the autophosphorylation of the β subunits and subsequently the phosphorylation of proteins inside the cell known as insulin receptor substrates (IRS). The phosphorylation of the IRS activates a signal transduction cascade that leads to the activation of other kinases as well as transcription factors that mediate the intracellular effects of insulin.
The cascade that leads to the insertion of GLUT4 glucose transporters into the cell membranes of muscle and fat cells, and to the synthesis of glycogen in liver and muscle tissue, as well as the conversion of glucose into triglycerides in the liver, adipose, and lactating mammary gland tissue, operates via the activation, by IRS-1, of phosphoinositol 3 kinase (PI3K). This enzyme converts a phospholipid in the cell membrane by the name of phosphatidylinositol 4,5-bisphosphate (PIP2), into phosphatidylinositol 3,4,5-triphosphate (PIP3), which, in turn, activates protein kinase B (PKB). Activated PKB facilitates the fusion of GLUT4-containing endosomes with the cell membrane, resulting in an increase in GLUT4 transporters in the plasma membrane. PKB also phosphorylates glycogen synthase kinase (GSK), thereby inactivating this enzyme. This means that its substrate, glycogen synthase (GS), cannot be phosphorylated, and remains dephosphorylated, and therefore active. The active enzyme, glycogen synthase (GS), catalyzes the rate-limiting step in the synthesis of glycogen from glucose. Similar dephosphorylations affect the enzymes controlling the rate of glycolysis leading to the synthesis of fats via malonyl-CoA in the tissues that can generate triglycerides, and also the enzymes that control the rate of gluconeogenesis in the liver. The overall effect of these final enzyme dephosphorylations is that in the tissues that can carry out these reactions, glycogen and fat synthesis from glucose are stimulated, and glucose production by the liver through glycogenolysis and gluconeogenesis is inhibited. The breakdown of triglycerides by adipose tissue into free fatty acids and glycerol is also inhibited.
After the intracellular signal that resulted from the binding of insulin to its receptor has been produced, the termination of signaling is then needed. As mentioned below in the section on degradation, endocytosis, and degradation of the receptor bound to insulin is the main mechanism to end signaling. In addition, the signaling pathway is also terminated by the dephosphorylation of the tyrosine residues in the various signaling pathways by tyrosine phosphatases. Serine/Threonine kinases are also known to reduce the activity of insulin.
The structure of the insulin–insulin receptor complex has been determined using the techniques of X-ray crystallography.
Physiological effects
Effect of insulin on glucose uptake and metabolism. Insulin binds to its receptor (1), which starts many protein activation cascades (2). These include translocation of Glut-4 transporter to the plasma membrane and influx of glucose (3), glycogen synthesis (4), glycolysis (5), and triglyceride synthesis (6).
The insulin signal transduction pathway begins when insulin binds to the insulin receptor proteins. Once the transduction pathway is completed, the GLUT-4 storage vesicles become one with the cellular membrane. As a result, the GLUT-4 protein channels become embedded into the membrane, allowing glucose to be transported into the cell.
The actions of insulin on the global human metabolism level include:
- Increase of cellular intake of certain substances, most prominently glucose in muscle and adipose tissue (about two-thirds of body cells)
- Increase of DNA replication and protein synthesis via control of amino acid uptake
- Modification of the activity of numerous enzymes.
The actions of insulin (indirect and direct) on cells include:
- Stimulates the uptake of glucose – Insulin decreases blood glucose concentration by inducing the intake of glucose by the cells. This is possible because Insulin causes the insertion of the GLUT4 transporter in the cell membranes of muscle and fat tissues which allows glucose to enter the cell.
- Increased fat synthesis – insulin forces fat cells to take in blood glucose, which is converted into triglycerides; a decrease in insulin causes the reverse.
- Increased esterification of fatty acids – forces adipose tissue to make neutral fats (i.e., triglycerides) from fatty acids; a decrease of insulin causes the reverse.
- Decreased lipolysis – forces reduction in conversion of fat cell lipid stores into blood fatty acids and glycerol; a decrease of insulin causes the reverse.
- Induce glycogen synthesis – When glucose levels are high, insulin induces the formation of glycogen by the activation of the hexokinase enzyme, which adds a phosphate group in glucose, thus resulting in a molecule that cannot exit the cell. At the same time, insulin inhibits the enzyme glucose-6-phosphatase, which removes the phosphate group. These two enzymes are key to the formation of glycogen. Also, insulin activates the enzymes phosphofructokinase and glycogen synthase which are responsible for glycogen synthesis.
- Decreased gluconeogenesis and glycogenolysis – decreases the production of glucose from noncarbohydrate substrates, primarily in the liver (the vast majority of endogenous insulin arriving at the liver never leaves the liver); decrease of insulin causes glucose production by the liver from assorted substrates.
- Decreased proteolysis – decreasing the breakdown of protein.
- Decreased autophagy – decreased level of degradation of damaged organelles. Postprandial levels inhibit autophagy completely.
- Increased amino acid uptake – forces cells to absorb circulating amino acids; a decrease in insulin inhibits absorption.
- Arterial muscle tone – forces arterial wall muscle to relax, increasing blood flow, especially in micro arteries; a decrease of insulin reduces flow by allowing these muscles to contract.
- Increase in the secretion of hydrochloric acid by parietal cells in the stomach.
- Increased potassium uptake – forces cells synthesizing glycogen (a very spongy, “wet” substance, that increases the content of intracellular water, and its accompanying K+ ions) to absorb potassium from the extracellular fluids; lack of insulin inhibits absorption. Insulin’s increase in cellular potassium uptake lowers potassium levels in blood plasma. This possibly occurs via insulin-induced translocation of the Na+/K+-ATPase to the surface of skeletal muscle cells.
- Decreased renal sodium excretion.
Insulin also influences other body functions, such as vascular compliance and cognition. Once insulin enters the human brain, it enhances learning and memory and benefits verbal memory in particular. Enhancing brain insulin signaling by means of intranasal insulin administration also enhances the acute thermoregulatory and glucoregulatory response to food intake, suggesting that central nervous insulin contributes to the coordination of a wide variety of homeostatic or regulatory processes in the human body. Insulin also has stimulatory effects on gonadotropin-releasing hormone from the hypothalamus, thus favoring fertility.
Degradation
Once an insulin molecule has docked onto the receptor and affected its action, it may be released back into the extracellular environment, or it may be degraded by the cell. The two primary sites for insulin clearance are the liver and the kidney. The liver clears most insulin during first-pass transit, whereas the kidney clears most of the insulin in the systemic circulation. Degradation normally involves endocytosis of the insulin-receptor complex, followed by the action of an insulin-degrading enzyme. An insulin molecule produced endogenously by the beta cells is estimated to be degraded within about one hour after its initial release into circulation (insulin half-life ~ 4–6 minutes).
Regulator of endocannabinoid metabolism
Insulin is a major regulator of endocannabinoid (EC) metabolism and insulin treatment has been shown to reduce intracellular ECs, the 2-arachidonylglycero(2-AG) and anandamide (AEA), which correspond with insulin-sensitive expression changes in enzymes of EC metabolism. In insulin-resistant adipocytes, patterns of insulin-induced enzyme expression are disturbed in a manner consistent with elevated EC synthesis and reduced EC degradation. Findings suggest that insulin-resistant adipocytes fail to regulate EC metabolism and decrease intracellular EC levels in response to insulin stimulation, whereby obese insulin-resistant individuals exhibit increased concentrations of ECs. This dysregulation contributes to excessive visceral fat accumulation and reduced adiponectin release from abdominal adipose tissue, and further to the onset of several cardiometabolic risk factors that are associated with obesity and type 2 diabetes.
Hypoglycemia
Hypoglycemia, also known as “low blood sugar”, is when blood sugar decreases to below-normal levels. This may result in a variety of symptoms including clumsiness, trouble talking, confusion, loss of consciousness, seizures, or death. A feeling of hunger, sweating, shakiness, and weakness may also be present. Symptoms typically come on quickly.
The most common cause of hypoglycemia is medications used to treat diabetes mellitus such as insulin and sulfonylureas. Risk is greater in diabetics who have eaten less than usual, exercised more than usual, or have drunk alcohol. Other causes of hypoglycemia include kidney failure, certain tumors, such as insulinoma, liver disease, hypothyroidism, starvation, an inborn error of metabolism, severe infections, reactive hypoglycemia, and several drugs including alcohol. Low blood sugar may occur in otherwise healthy babies who have not eaten for a few hours.
Diseases and syndromes
There are several conditions in which insulin disturbance is pathological.
- Diabetes mellitus – a general term referring to all states characterized by hyperglycemia. It can be of the following types:
- Type 1 – autoimmune-mediated destruction of insulin-producing β-cells in the pancreas, resulting in absolute insulin deficiency
- Type 2 – either inadequate insulin production by the β-cells or insulin resistance or both because of reasons not completely understood.
- there is a correlation with diet, with a sedentary lifestyle, with obesity, with age, and with metabolic syndrome. Causality has been demonstrated in multiple model organisms including mice and monkeys; importantly, non-obese people do get Type 2 diabetes due to diet, sedentary lifestyle, and unknown risk factors.
- it is likely that there is genetic susceptibility to develop Type 2 diabetes under certain environmental conditions
- Other types of impaired glucose tolerance, IFG IPPG
- Insulinoma – a tumor of beta cells producing excess insulin or reactive hypoglycemia.
- Metabolic syndrome – a poorly understood condition first called Syndrome X by Gerald Reaven. It is not clear whether the syndrome has a single, treatable cause, or is the result of body changes leading to type 2 diabetes. It is characterized by elevated blood pressure, dyslipidemia (disturbances in blood cholesterol forms and other blood lipids), and increased waist circumference (at least in populations in much of the developed world). The basic underlying cause may be the insulin resistance that precedes type 2 diabetes, which is a diminished capacity for insulin response in some tissues (e.g., muscle, fat). It is common for morbidities such as essential hypertension, obesity, type 2 diabetes, and cardiovascular disease (CVD) to develop.
- Polycystic ovary syndrome – a complex syndrome in women in the reproductive years where anovulation and androgen excess are commonly displayed as hirsutism. In many cases of PCOS, insulin resistance is present.
Fast-acting insulin: It begins operating around a quarter-hour when infusion and topnotch at roughly one hour nonetheless keeps on operating for 2 to four hours. This is often generally taken before supper and however a long hormone.
Short-acting insulin
It begins operating roughly half-hour when infusion and crests at around a pair of to three hours but can persevere operating for 3 to 6 hours. It’s generally given before supper and however a long hormone.
Moderate acting insulin
It begins operating roughly a pair of to four hours when infusion and pinnacles are around four to twelve hours when the fact is and keeps on toiling for 12-18 hours. It’s typically taken double per day and however a fast or short-acting hormone.
Long-acting insulin
It begins operating after a couple of hours when infusion and works for roughly twenty-four hours. On the off probability that vital, typically used in mix with a quick or short-acting hormone.
Insulin may be given by a syringe, infusion pen, or associate hormone siphon that conveys a perpetual progression of the hormone.